Osteoarthritis of the knee (gonarthrosis) is damage to the knee joint primarily inflammatory, which leads to wear of the cartilage layer of the knee joint and eventually to the destruction of cartilage, deformation of the knee and limitation. It is therefore important to be able to recognize the disease and know how and how it is treated.
Osteoarthritis of the knee (gonarthrosis is also called – from the Greek "drive" – knee) is a progressive, degenerative-dystrophic lesions of the cartilage lining the surface of the joint, which leads to disruption of its work and pain.
The causes of osteoarthritis of the knee
Gonarthrosis is divided into primary (caused by yourself) and secondary, which occurs as a consequence of other diseases of the knee joint.
Primary
Osteoarthritis primary (genuinny) is arthritis that begins no discernible reason and striking unaltered articular cartilage in many joints at the same time. Occurs more frequently in persons older than 40 years. It is also proven that women more often than men suffer from arthrosis of the knee and hand joints.
What causes primary osteoarthritis, has not been fully elucidated, but most likely, it leads to violations of metabolism. This causes changes of biochemical reactions that occur in cartilage. Eventually she collapses, degenerates and accumulates salt. The surface of the knee joint varies with the structure of the cartilage, resulting in knee accumulates fluid and there is a cyst Becker.
Secondary
It is the result of diseases or injuries of the joints, in their clinical manifestations does not differ from the primary. Develops in almost any joints.
Secondary osteoarthritis occurs for the following reasons:
- the inflammatory process of immune or infectious origin;
- dysplasia or traumatic injuries of the meniscus or knee (miniscope);
- intra-articular fractures of the bones forming the knee joint;
- rheumatoid arthritis;
- bone tumors;
- ankylosis spondylitis;
- arthritis that occurs in Paget's disease.
Symptoms

Symptoms of osteoarthritis include the following:
- pain in the feet, knees, hip joints, lower back;
- stiffness, stiffness and crunching in the joints;
- the pain after sleeping or a long stay in one position;
- swelling of the joints;
- aches when weather changes;
- pain in joints after exertion;
- trauma – fractures, dislocations, and damage to the meniscus;
- high loads;
- overweight and obesity;
- weak ligaments – ligaments are loose;
- violation of metabolic processes in the body;
- stress.
Deformity of the joint
Deformation of the joint is changing the shape of the joint, caused by the displacement of the mating ends of the bones in dislocation, the development of the pathological joint tissue growths. Most often deformation of the exposed joints of the hands, feet, legs.
Joint deformity is usually the result of complex metabolic disorders in periarticular, bone, or cartilage tissue, where they tend to accumulate in this atypical localization and concentration of the substance.
A consequence of the deformation of the joints is often fusion of the joints, bony growths, subluxations of the joints and injuries of the musculo-ligamentous apparatus.
In relation to this accompanying symptom of osteoarthritis apply symptomatic treatment, but a holistic approach aimed at eliminating the disease as a whole demonstrates greater efficacy and prevents the recurrence.
Diagnosis of deformity of the joints occurs independently from the overall diagnosis. It is the basis of further investigation and General conclusions. Objective examination of the joints allows to determine their configuration, swelling, tenderness at palpation and movement, the amount of active and passive movements in the joints and changes in the skin and subcutaneous tissue in the joints.
Limitation of joint mobility
Distinguish different degrees of mobility limitation from light, barely noticeable violate the usual range of motion, to a complete loss of mobility.
According to the degree of limiting the mobility of the joint are:
- Ankylosis – complete immobility in the diseased joint.
- Rigidity – saved only a small range of motion. For example, a small rocking motion. On examination, rigidity must be differentiated from ankylosis.
- Contracture – a limitation persistent and significant, but, nevertheless, there remains some scope of movements in the joint. To diagnose the volume of movements using a simple inclinometer.
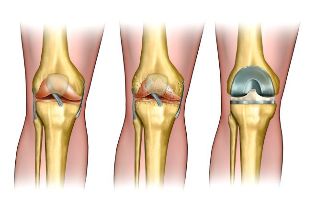
The degree of arthrosis of the knee joint
First. In this case, the disease is characterized by slight pain when performing active movements. May accumulate synovial fluid in the joint cavity, which leads to the formation of Baker's cyst. Pain occur during movement, but are at rest. The cartilage tissue is damaged, but externally, the deformation of the joint invisible.
Second. There is a narrowing of the joint space, the cartilage is damaged to a large extent. In the picture obtained during radiography, it is possible to notice the growth of bones. Acute pain is accompanied by any movement which involved the knee joint. At rest the unpleasant sensations are, but then appear again. The pain adds a distinctive crunch when making extensor movements.
Third. Sometimes the cartilage becomes thin, the formation of bare areas of bone. On the radiograph clearly seen a large number of osteophytes – salt deposits in the joint cavity. In addition, there may be discovered free of the body.
Possible complications and consequences of a knee
Knee osteoarthritis is a degenerative disease that eventually progresses. Joint pain and stiffness become so severe that the patient is unable to cope with daily Affairs. Some people lose the ability to work when arthritis reaches to a point that a doctor only recommends surgery for joint replacements.
If you ignore symptoms of the disease and not spend a timely treatment, the risk of complications is quite high.
To the possible consequences of the running of osteoarthritis include:
- critical deformation of the joint, its complete destruction;
- global limited mobility;
- the occurrence of intervertebral hernias;
- the decline in the quality of life, loss of working capacity.
What kind of doctor treats?
This can be a primary care physician, surgeon, podiatrist. As necessary, appoint the advice of a rheumatologist. A rheumatologist will examine You, establish a precise diagnosis and determine exactly which joints are affected. Will prescribe laboratory and instrumental methods of diagnosis.
Only through a full examination, the specialist will be able to answer the main question: what stage of gonarthrosis in a patient, and what treatment he needs.
In the presence of concomitant pathologies in the spinal column is required to consult a neurologist and vertebrologist. These professionals prescribe rehabilitation treatment, which eliminates the pain syndrome due to the infringement of nerve fibers in the intervertebral discs.
Diagnosis
Of joint disease resembling arthritic, occur in many other diseases, and ignorant people are often mistaken in defining the disease. Therefore, in any case, do not try to establish a diagnosis on their own.
Instrumental examination
Diagnostic radiology is the most popular and important method because of its simplicity, accessibility and high information content. Images are usually performed in two projections, lateral and frontal, but if necessary can use a variety of specific installation.
Ultrasound is considered to be quite promising direction, which allows to detect the liquid, to assess the pathologies of soft tissues, and to visualize the cartilage and joint surfaces. The advantages of this method over radiography is the ability to change the position of the sensor, and the lack of need of strict positioning of the patient for obtaining the standard projections.
MRI and CT provide a large amount of information, and the ability to obtain three-dimensional image of the study area.
Laboratory tests
When osteoarthritis pathological changes occur mainly in the articular cartilage and in subchondral bone, synovial membrane, and other soft tissues of the joint. Because of the possibility to directly probe the structure are limited, the most important sources for collection of the bio-markers are blood, urine and synovial fluid.
In most cases, patients with knee arthritis there are no changes in the blood and urine tests, except in cases of synovitis with significant effusion, when there is increased erythrocyte sedimentation rate, hypergammaglobulinemia, increased level of acute phase CRP, fibrinogen, etc. in the study of synovial fluid in significant differences from the normal indicators do not reveal.
In recent years there has been an intensive search for possible biological markers (BM) degradation and repair joint tissue (mostly cartilage and bone). BM reflect dynamic changes, are predictors of prognosis of osteoarthritis and the markers of the effectiveness of pathogenetic therapy. The discovery of new and deeper study of the famous BM will allow to better understand the mechanisms of pathogenesis of osteoarthritis.
However, the main objective of the use of biological markers of cartilage metabolism – evaluation of the chondroprotective properties of drugs and monitoring of treatment with drugs belonging to the group of "disease-modifying".
Treatment of osteoarthritis of the knee
The treatment of arthritis, to put it mildly, not the easiest task. So before You start your uphill battle with this disease, be sure to find a good doctor, be surveyed in him and with him make a treatment plan.
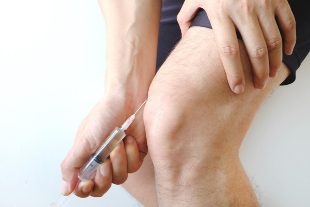
Drugs
The most commonly prescribed medications for inflammation and pain in osteoarthritis of the knee joint is anti-inflammatory drugs non-steroidal nature. Medications are effective in inflammatory processes, accompanied by synovitis. In addition, the above-mentioned drugs relieve pain. However, they do not treat the disease itself.
When taking non-steroidal anti-inflammatory drugs should comply with all recommendations of the doctor, as such drugs have an impressive number of side effects, especially with prolonged use.
Chondro – is a class of medicines that restore bone and cartilage. When taking chondroprotectors it is worth considering that these drugs are maximally effective in the complex treatment of the disease.
Vasodilator drugs are also prescribed in the treatment of osteoarthritis. Using them is possible to restore the blood circulation in the joint, as well as relieve spasms of the small blood vessels.
In an analgesic most commonly used as an ointment or compresses with a warming effect. When you need quick relief can be shown intra-articular injection of corticosteroids.
Surgery
Puncture (minimally invasive intervention). This method is used for diagnosing the disease. The joint capsule insert the needle, taking some of the liquid. This allows to obtain material for analyses, to reduce the load on the capsule, if necessary, enter the corticosteroids directly to the site of inflammation.
Arthroscopy. Provides an introduction to the special office of the arthroscope through the incisions in the skin. The method allows to thoroughly inspect the joint, and remove separated fragments of cartilage, eliminating the causes of inflammation and pain.
Periarticular osteotomy. The method consists in sawing the bone with subsequent fixation them from a different angle. The operation reduces the load on the joint and eliminate pain for a longer period. Despite its effectiveness, this type of surgery is used infrequently – too much of a burden on the patient and long term rehabilitation.
The endoprosthesis. In cases where other treatments have not helped, and the disease is completely or almost completely destroyed the joint are replaced by prostheses made of plastic, metal or ceramic.
Arthroplasty is a heavy and expensive operation, requiring long-term rehabilitation. Many patients for several months after surgery pain. However, this method often is the only alternative to immobility of the patient. The life of a modern prosthesis reaches twenty years, and all these years the patient may live a full life.

Recommended diet
Diet necessary in the first place in order to control their weight. It is proved that osteoarthritis often develops and harder just tolerated in people with excess weight, therefore:
- limit alcohol, fatty foods, semi-finished products;
- control the power mode;
- reduce the amount of salt;
- reduce the amount of sweets;
- eat more vegetables and fruits (preferring seasonal).
Prevention of osteoarthritis
The main measures to prevent the development of osteoarthritis are:
- reduction of overweight;
- the increase in locomotor activity;
- proper nutrition;
- adherence to the principles of a healthy lifestyle.
Maintaining a healthy lifestyle will strengthen Your body, improve the condition of cartilage, joints and bones. It is necessary to refuse from alcohol and Smoking. A lot of time outdoors, to experience less stress and anxiety, lots of good mood and positive.
Arthritis – a disease that is not cured completely, however, its development can be stopped, if the time to pay attention to their health and to start treatment. Therapy can reduce, or even remove completely some of the symptoms, which greatly facilitates the life of a sick person.
















