Osteochondrosis is a chronic inflammatory disease occurring on a background of constant destruction of the vertebrae and intervertebral discs. Depending on the localization of vertebral structures are subjected to degenerative changes, there are thoracic, lumbo sacralis pathology, as well as the neck. Leading symptoms of degenerative disc disease and pain syndrome, the severity of which increases with physical exertion, stiffness. The clinical picture often present vertebral symptoms: headaches, racing blood pressure, decreased visual acuity and hearing.
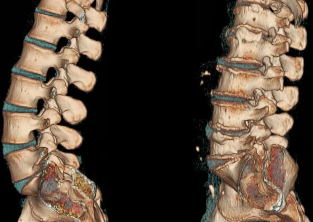
The diagnosis put on the basis of results of instrumental investigations — x-ray, MRI, CT. In the treatment of degenerative disc disease used drugs a variety of clinical and pharmacological groups. To enhance their clinical effectiveness offers physiotherapy and massage treatments. One of the main methods of treatment and prevention is physical therapy.
The mechanism of disease development
The pathogenesis of degenerative disc disease is the loss of nucleus pulposus the nucleus of their hydrophilic properties. This fluid structure is composed of connective tissue fibers and a gelatinous substance. As they Mature the person is a reduction of the vascular bed in each disc between the vertebrae. Admission to it of nutrients occurs diffusely, that is, the principle of spontaneous equalization of concentrations. This explains the impossibility of the full restoration of cartilage tissue after injury or excessive physical loads on the spine.
Processes exacerbate degenerative disc disease hormonal changes and unbalanced diet. Cartilage does not receive sufficient for their normal functioning amount of nutrients, which causes the following violations of their structure and properties:
- lost strength and elasticity;
- the shape, texture and configuration.
The intervertebral discs are flattened, and the fibrous rings formed the radial cracks. This causes a decrease in the distance between adjacent vertebrae. Gradually in the pathological process involves the connective tissue of the fibrous ring, ligaments. In response to the disintegration of the tissues, the immune system starts producing antibodies, which leads to aseptic inflammation and formation of edema in the joints and nearby soft tissues. Capsules of the joints are stretched, so the intervertebral discs no longer a reliable fixation of the vertebrae. And the instability of intervertebral segments increases the likelihood of infringement of the nerve root or compression of a blood vessel. This often occurs with cervical osteochondrosis and becomes the cause of his severe symptoms.
Causes and predisposing factors
On the state of the intervertebral discs affects a lowered tonus of skeletal muscles of the vertebral column. Irrational, asymmetric muscle function occurs during prolonged human presence in not a physiological situation, for example, with his head down while working at the computer. Trigger destruction of the cartilage tissue can permanent wearing heavy bags on one shoulder sleeping on a soft mattress and high pillow.
Accelerate the destruction of intervertebral disks is also following external and internal negative factors:
- endocrine and metabolic disorders;
- of infectious diseases, especially chronic;
- previous spinal injuries (compression fractures, bruises);
- frequent overcooling;
- the presence of systemic or degenerative diseases — gout, psoriatic, rheumatoid arthritis, osteoarthritis, osteoporosis.

If a person has bad habits, he is at risk. Smoking and excessive alcohol worsen the condition of blood vessels lead to insufficient circulation and nutritional deficiency in cartilage disks.
In the presence of flat feet or clubfoot is significantly increased risk of developing osteoarthritis of any location. Such congenital or acquired defects are the cause of increasing the load on the spine due to the inability to provide proper cushioning with support. Predisposing factor pathology is obesity.
The deposition of fatty tissues in various parts of the body can be difficult to maintain the balance that leads to exposure to excessive loads on the intervertebral joints.
The clinical picture
The first clinical manifestation of a cervical, thoracic or lumbar degenerative disc disease — back pain. During relapses it is penetrating, radiating to nearby parts of the body. The slightest movement leads to increased severity of pain. Response of a man is making the forced position in which the intensity of the discomfort is minimal:
- people with cervical osteochondrosis prefer to turn to the side not the head and the entire body;
- breast pathology when man is afraid even to do a full inhale, as it causes sharp pain in the thoracic spine;
- patients with lumbar osteochondrosis with difficulty sit down, stand up and walk because of the infringement of spinal nerve.
Most patients complain about the doctor for a dull persistent pain and feeling of stiffness in the limbs in the morning. This requires additional differential diagnosis to exclude myositis (inflammatory process in the skeletal muscles of the back) and osteoarthritis. The cause of the aching, crushing pain — compensatory stress the muscle tissues to stabilize the affected vertebral-motor segment. Permanent pain syndrome weak or moderate intensity is occurring because of significant stretching of the intervertebral disc and the development of aseptic inflammation.
For osteoarthritis a specific localization, specific symptoms. For example, when lumbar pathology often occurs sciatica — a pain in the lumbar region and back of the thigh. Thoracic osteochondrosis clinically manifested visceral pain in cardiac region, right hypochondrium and abdomen, numbness, increased sensitivity of the skin, the crunch of vertebrae. But the most pronounced and varied symptoms different pathology affects the cervical intervertebral discs.
As a result of displacement of the vertebrae and formation of osteophytes compressed by the vertebral artery supply brain cells providing them with oxygen. People suffering from lack of coordination of movements, tinnitus, headaches, hypertension.
What could be if untreated
Most complications of degenerative disc disease arise from the formation of herniated disc. It is formed at the offset of this spinal structure back that leads to rupture of the posterior longitudinal ligament. The disk becomes more unstable, and part of it protrudes into the spinal canal. Considered a ruptured hernia, if in the process of its formation along with a disc in the channel penetrates his purposee core.
This pathological condition of the vertebral structures predisposes to the spinal cord compression and development of discogenic myelopathy. Clinically it is manifested in torpor, weakness of some muscle groups of the legs or hands, paresis, muscle atrophy, altered tendon reflexes. There may also be disorders of emptying the bladder and (or) intestinal. As a result of formation of a herniated disc compressed the arteries that feed the spinal cord. Formed in ischemic areas, which killed all the nerve cells. A so-called neurological deficit — violated movement, decreased sensitivity, upset trophic.

Treatment
Osteochondrosis can't be completely cured, as it is not yet synthesized drugs, the reception of which would help to repair damaged intervertebral discs and vertebrae. But in a therapeutic scheme must be included chondroprotectors — symptomatic treatment delayed effects. Preference is given to drugs with active ingredients chondroitin sulfate and (or) glucosamine sulfate (hydrochloride).
The clinical efficacy of these drugs is confirmed by the results of years of research. In the long admission (from 3 months to 2 years) means there is a partial regeneration of cartilage and other connective tissue structures — ligaments, tendons, burs. Accumulation in the intervertebral discs of glucosamine and chondroitin they begin to exert a pronounced analgesic, antiedematous, anti-inflammatory effect. This allows lower doses of NSAIDs, corticosteroids, muscle relaxants, thereby reducing the pharmacological load on the body.
The joint Supplement ineffective the irregular employment or their use for the treatment of osteoarthritis grade 3, when there is a significant destruction of the cartilage.
To eliminate the symptoms, usually occurs in cervical or thoracic degenerative disc disease, used drugs to improve blood circulation, nootropics, the drug, improves microcirculation of the labyrinth, used in pathology of the vestibular apparatus.
Optionally, in the therapeutic scheme included antidepressants and anticonvulsants.
In the treatment of osteoarthritis applied physiotherapy: UHF-therapy, magnetic therapy, laser therapy. Used reflexology, massage, exercise therapy, hirudotherapy, swimming, yoga. With the ineffectiveness of conservative treatment, the patient, surgical intervention. Practiced puncture vaporization of the disc, a laser reconstruction or replacement of the implant.
















